Release date: 2016-04-01
Human immunodeficiency virus (HIV), an AIDS (AIDS, acquired immunodeficiency syndrome) virus, is a virus that causes defects in the human immune system. In 1983, HIV was first discovered in the United States. It is a lentivirus that infects cells of the human immune system and is a type of retrovirus.
By destroying the body's T lymphocytes, HIV blocks cellular and humoral immune processes, causing the immune system to paralyze, causing various diseases to spread in the human body and eventually leading to AIDS. Due to the extremely rapid variation of HIV, it is difficult to produce a specific vaccine, and there is no effective treatment method to date, which poses a great threat to human health.
To date, only one "Berlin patient" Timothy Ray Brown has been reported worldwide to be considered to have completely cured HIV. In 2007, after his leukemia treatment in a German hospital, Brown's HIV virus completely disappeared. In the treatment of leukemia, Brown first received radiotherapy to kill cancer cells and stem cells that make cancer cells in the bones. Then, through bone marrow transplantation, a healthy person's bone marrow was implanted to produce new blood cells. After receiving treatment, Mr. Brown's leukemia improved, and the level of HIV in the body also dropped sharply, and the instrument could not detect it. It was gratifying that until now, Brown did not detect the HIV virus, and even more surprising is the ordinary. He has not taken antiretroviral drugs for HIV patients. But then scientists used the treatment in monkeys and HIV patients with lymphoma, and the results did not cure HIV. According to this, scientists believe that the person who donated bone marrow to Mr. Brown played an indispensable role, because the donor's gene CCR5 has a rare mutation.
This is just an episode. After all, there is only one case and it cannot be copied. The persistence and tenacity of HIV infection are well documented. Significant medical advances have changed HIV/AIDS from a terminal illness to a controlled disease since the 1980s. Current antiretroviral drugs are usually used in combination, and their types include entry inhibitors, which function to interfere with HIV binding to host cells; nucleoside reverse transcriptase inhibitors, which function to inhibit HIV integration into host cell DNA; integrase Inhibitors, whose function is to block a key HIV viral enzyme, integrase; a protease inhibitor, which functions to block a protease that plays a key role in the maturation of HIV virus particles. However, no vaccines, drugs or therapies have been able to permanently cure HIV-infected patients.
1. Science: A major breakthrough in HIV! The most detailed three-dimensional structure of HIV envelope in history has been released!
This study is the first to resolve a high-resolution structural map of the HIV Env trimer in its natural state, in which HIV invades host cells using Env trimers. Image courtesy of The Scripps Research Institute.
Imagine an airplane ready to land. Next, imagine the airport covered with a lot of barbed wire. This is a similar challenge faced by antibodies in humans trying to neutralize HIV.
Andrew Ward, associate professor of the paper and associate professor of The Scripps Research Institute (TSRI), said, "The human immune system can produce an immune response, but these reactions cannot effectively attack the virus."
Ideally, the antibody is capable of targeting the Env trimer of HIV, the three loosely linked proteins, extending from the HIV envelope to the outside, allowing the virus to fuse with the host cell, thereby infecting them. This "fusion machinery" is also a very important target because its structure is highly conserved, which means that the same vulnerable sites exist in many HIV strains. The antibody at the site is likely to be a broad-spectrum neutralizing antibody. Unfortunately, a sugar molecule protector called glycan prevents many antibodies from reaching this region.
In order to develop a vaccine against HIV, scientists need to map the structure of these polysaccharides in detail to reveal the small loopholes in the protection, so that antibodies can cross these small loopholes and neutralize this. HIV.
However, this HIV Env trimer is extremely unstable, making it difficult for scientists to capture good structural images. Partly because of this limitation, previous studies by TSRI and other agencies have only obtained truncated Env trimers or high-resolution structural maps of Env trimers that have become stable by mutation. Prior to this, no one was able to observe this trimer and its polysaccharide defense structure in its natural state.
In a new study, TSRI researchers resolved high-resolution structural images of HIV proteins responsible for identifying and infecting host cells. The results of the study were published in the March 4, 2016 issue of Science, titled "Cryo-EM structure of a native, fully glycosylated, cleaved HIV-1 envelope trimer".
This study is the first to resolve the structural picture of the HIV protein called envelope glycoprotein trimer (hereinafter referred to as Env trimer) in its natural state. These also include a detailed map of the fragile sites at the bottom of the protein, as well as a map of antibody binding sites capable of neutralizing HIV.
2. eLife: Revealing the two mutation patterns of HIV-producing genes
Since the first appearance of HIV/AIDS in 1981, the treatment of this disease has changed dramatically. When antiretroviral drugs were first used, almost every patient developed resistance during the first year of drug use. However, resistance is now very rare and HIV patients are often able to maintain healthy lives.
After analyzing the 6717 patient records, Alison Feder and colleagues from Stanford University in the United States found that in patients, HIV acquires resistance in two different ways, which may represent the effectiveness of the medication taken by the patient. The virus first overcomes the effects of the drug by maximizing its own genetic diversity. However, over time, the virus sacrifices genetic diversity to develop resistance to advanced, more widely and effective therapeutics.
By combining historical HIV records with the Stanford University HIV resistance database, the researchers found that two specific mutations can be used as indicators to evaluate treatment feasibility.
In some cases, HIV develops resistance by acquiring genetic polymorphisms in the host. The higher incidence of mutations in the HIV population gives the virus more opportunities to simultaneously produce multiple drug-resistant mutations that simultaneously spread throughout the patient's HIV population, thus maintaining a high diversity.
Another mode of mutation is that HIV successfully produces only a single drug-resistant mutation. When this single mutation spreads throughout the body, HIV becomes genetically homogenous. In the HIV population, the situation in which a single mutation produces resistance is relatively rare.
Discovering how HIV responds to different therapeutic drugs will help scientists determine the effectiveness of a drug and help scientists develop new therapeutic drugs. ( eLife , 14 February 2016, doi: 10.7554/eLife.10670 )
3. HIV-resistant strains invalidate the preventive drug Truvada
Doctor at the Maple Leaf Clinic in Toronto, Canada, last week at the International Conference on Retroviruses and Opportunistic Infections in Boston, USA, reported that a 43-year-old Canadian man, despite taking 24 months of anti-HIV drug Truvada It is still diagnosed as HIV positive in the near future.
The US Food and Drug Administration (FDA) approved the launch of the drug in 2012 to ensure safe sex to prevent HIV infection. Truvada is a combination of two different drugs (emtricitabine and tenofovir). Together, the two drugs inhibit an enzyme (RdRp) that helps the HIV virus complete RNA-to-DNA reverse transcription. Without this enzyme, HIV cannot replicate in the body, so drugs can prevent the spread of the virus.
This does not mean that the drug Truvada does not work for HIV. This just means that Truvada is not 100% effective, which may be disappointing, but not surprising. Because no treatment or prevention method will be foolproof. Measures such as pre-exposure prophylaxis with HIV can still prevent the spread of HIV.
4. Lancet Infect Dis: Shocked! HIV tenofovir resistance is very common
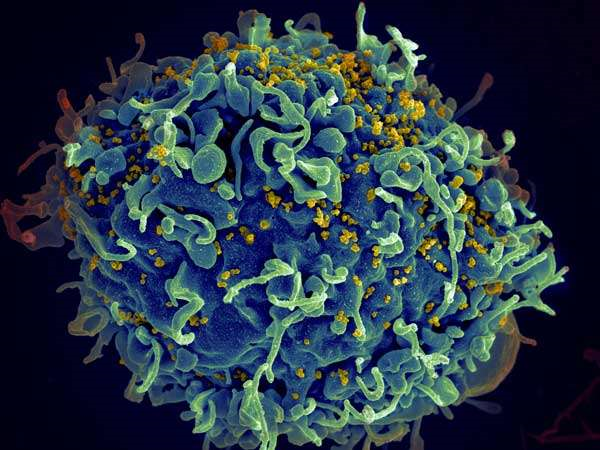
Image courtesy of HIV (yellow) infected with immune cells, images from Seth Pincus, Elizabeth Fischer and Austin Athman/National Institute of Allergy and Infectious Diseases/National Health Center.
Tenofovir is an antiretroviral drug that plays a vital role in most modern HIV treatment and prevention strategies. However, according to a large study funded by the Wellcome Trust, HIV resistance to tenofovir is becoming surprisingly and worryingly common.
The study was conducted by researchers from Stanford University in the United States and the School of Health and Tropical Medicine in London, England. The researchers studied 1,926 HIV patients around the world who, despite taking antiretroviral drugs, still have uncontrolled HIV. The researchers found that tenofovir-resistant HIV strains were present in 60% of sub-Saharan African patients, compared with 20% of patients treated in Europe. About two-thirds of patients with tenofovir-resistant HIV strains also develop resistance to two other drugs in their treatment regime. The results of the study were published online January 28, 2016 in the journal Lancet Infectious Diseases.
5. PNAS: A new barrier to HIV treatment strategies
The HIV-1 virus, imaged by J Roberto Trujillo/Wikipedia.
This is a mixed story: the researchers have made a new discovery about HIV that will help redirect the treatment strategy to the latent HIV virus pool, which is good news. The bad news is that they found that cloned expanded HIV-infected cells persisted and produced new viruses for many years in a patient undergoing combination antiretroviral therapy (cART). Therefore, any method of treating HIV infection will have to attack these cells in order to permanently remove the virus.
In a current new study, a large international research team first confirmed the presence of a contagious HIV-1 virus pool in CD4+ T cells, and these HIV-1 infected T cells have clonal expansion capabilities, ie A single cell is capable of producing a population of cells. These T cell clones contain live viruses that can begin to proliferate once cART treatment is stopped.
It took more than a decade to get this conclusion. These findings were derived from a study of an HIV-positive patient who was first diagnosed in 2000. The researchers performed virology, immunology, and diarrhea analysis from the start of cART treatment in this African-American male. After 13 years, the patient died of cancer. Prior to the publication of this paper, it was not known whether these same viruses found in the blood cells of patients were contagious. "These findings confirm that cells containing HIV-1 provirus that replicates [ie, HIV integrated into the host DNA] can be cloned, expanded, and persisted in vivo," they write, presenting new challenges for treating HIV infection. ."
6. JCI: Major Discovery! HIV not only targets T cells, but also targets macrophages.
In a research paper published in the International Journal of Clinical Investigation , researchers from the University of North Carolina School of Medicine found that HIV can infect macrophages and multiply in macrophages. Macrophages are A large white blood cell in the body's liver, brain, and connective tissue, the study found or could help develop new therapies for treating HIV infection.
Researcher Dr. Joseph Eron pointed out that this study clearly clarified that macrophages can be used as a site for replication of HIV virus. Macrophages are myeloid cells. In order to determine whether macrophages in tissues can be infected by HIV infection, Using a humanized myeloid mouse model, the researchers found that macrophages can maintain HIV replication in the absence of T cells, while HIV-infected macrophages can be distributed throughout the body. In many organizations, such as the brain. Viruses with replication potential can be recruited by infected macrophages from the model, while infected macrophages can also establish novel infections in new hosts. Studies have shown that macrophages may be infected as HIV. The real target to maintain and deliver this infection.
7. J Virol: How gut microflora affects HIV progression
HIV may be an intestinal disease. This concept makes it easy for us to ignore the sexual and blood-borne properties of the cause. In fact, HIV infects and kills CD4+ cells, and about two-thirds of T cells are located. In the lymphatic tissue of the intestine, where HIV spreads and spreads. In recent years, research on blood has attracted more and more scientists' attention, because blood can circulate throughout the body, and the intestine seems to be difficult to reach. Researchers can only study it through invasive methods. A good understanding of the environment of the intestine may help to understand the pathogenesis of the disease.
Recently, researchers from institutions such as the University of Washington said that HIV infection reduces the number and diversity of beneficial bacteria in the gut, while increasing its negative effects on the gut, which will promote an ecological imbalance in the gut. Ecological imbalance is a kind of interference phenomenon in the intestinal microbiome of the body, which can cause interference phenomenon of many different microbial groups, thus inducing different diseases of the body.
8. PLoS Pathog: When HIV invades your brain
A new study explains, in part, why HIV is often eliminated. Because the HIV virus is more "insidious" than we think. Researchers at Yale University School of Medicine and the University of North Carolina found that within four months of HIV infection, the HIV virus can break through the blood-brain barrier, enter the brain, and stabilize in the brain. After some time, these HIV viruses gradually mutate and begin to become different from those in the blood circulation system. However, anti-HIV drugs in the blood do not kill the HIV virus that is present in the brain. Thus, after a certain period of time, these surviving variant HIV viruses can have a large negative impact on the nervous system and mental health, such as causing brain atrophy.
9. J Leuk Biol: "Trojan Horse" that helps HIV enter the brain
Although everyone knows that HIV can enter the patient's brain at the beginning of infection, causing inflammation and memory problems, but how it happens is unknown. In a research paper published in the journal Journal of Leukocyte Biology , researchers from the Albert Einstein School of Medicine revealed that HIV can be expressed by an immune cell called mature monocytes. The proteins JAM-A and ALCAM come into the brain, so these two proteins may be a new drug target that inhibits HIV from entering the brain cells. Although there are few related studies, the researchers believe that this is a late development of new drugs. The blood-brain barrier provides new ideas for the treatment of HIV infection.
10. J Infect Dis: A New Approach to HIV Transmission
HIV-1 infection is transmitted primarily to children through sexual contact and motherhood. A series of clinical trials of vaccines and microbicides, while preventing the spread of HIV, have not been successful. New research shows that HIV-infected cells colonize HIV-infected male and female genital secretions and breast milk, and scientists are now trying to design HIV-infected cells in the secretions to prevent the spread of HIV.
Source: Bio Valley
Stainless Steel Triclover Clamp,Steel Triclover Clamp,Stainless Steel Solid End Cap,Stainless Steel Tank
Wenzhou Gaoya Light Industry Machinery Co.,ltd. , https://www.hongyafitting.com